

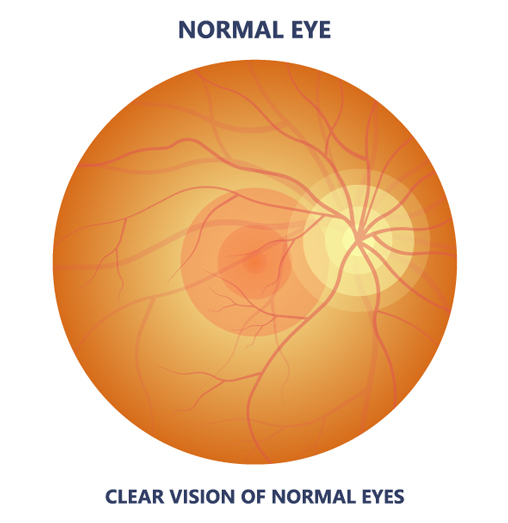
Age-related macular degeneration (AMD) is the most common cause of visual loss in Americans above 55 years of age and affects more than 10 million Americans. AMD is a chronic disease marked by the deterioration of the central portion of the retina which is the layer in the back of the eye that captures all the images we see and sends them via the optic nerve to the brain. The deterioration results in central visual loss. There are two main types of macular degeneration, dry and wet macular degeneration.
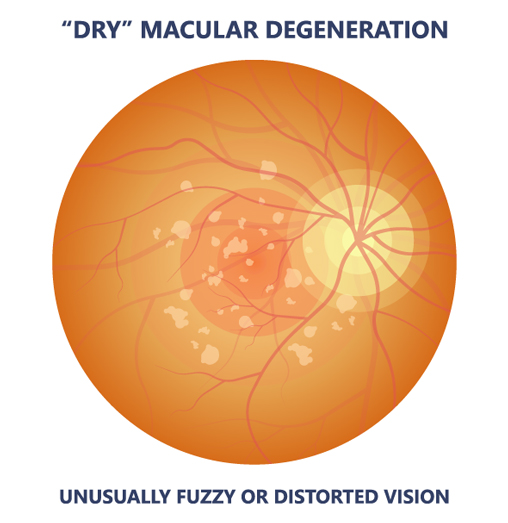
The most common type of macular degeneration is dry macular degeneration and it makes up 90% of all macular degeneration. This type is characterized by a slower decrease in central vision than wet macular degeneration. In this form, there is no fluid within the macula but there are yellow spots termed drusen under the retinal pigment epithelium, beneath the retina. These spots are the result of the accumulation of debris which should have been removed by other cells; this debris interferes with the function and metabolism of the light sensitive cells of the retina. Patients with early dry macular degeneration may have good vision but experience fluctuating vision, decreased brightness of colors, reduced night vision or illumination, and difficulty reading. Patients may also have difficulty with dark adaptation as when walking from a bright room to a dark room and may also have difficulty recognizing faces.
People with macular degeneration may also experience visual hallucinations, a common occurrence in AMD; this is called the Charles Bonnet syndrome.
No, not necessarily. About 50% of the population will show hard drusen and almost 100% the population above 50 will have at least one druse, but many will not develop macular degeneration. An examination by your doctor will help you better understand your risk and what to do about treatment.
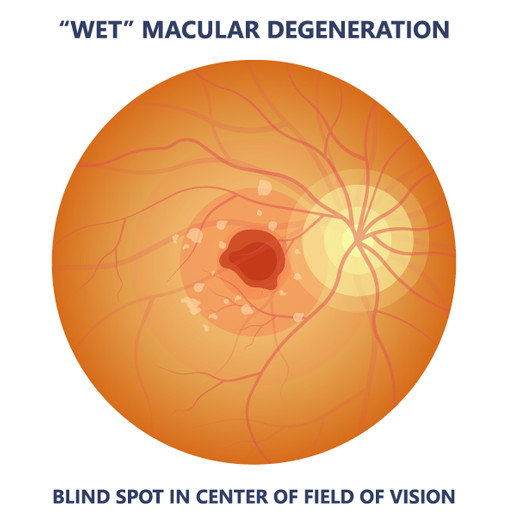
When the retina gets significantly degenerated, abnormal blood vessels grow under the retina and can leak fluid or bleed, causing distortion of central vision. Straight lines may look wavy or areas of vision can become blocked by blood; If left unattended, this bleeding can lead to scarring and total loss of central vision.
The risk of macular degeneration (AMD) increases with age. Other risk factors include:
Diet may play a role in the development of macular degeneration. A diet including citrus fruits, greens, and fish oil and low in its glycemic index (sugar) could help slow down the onset and progression of AMD. The following recommendations may be helpful to include in your diet, which could lead to a decreased risk of macular degeneration and/or a slower rate of progression. Always discuss this with your doctor before starting a regimen, as they may affect other conditions.

Carotenoids- can be used by the body to produce vitamin A which may slow age-related macular degeneration. They are present in carrots, spinach, kale, apricots, papaya and mango. Lutein and zeaxanthin are carotenoids that cannot be used to make Vitamin A, but may also be important to the health of your eyes. Lutein is found in egg yolks and dark, leafy greens and in fruits such as oranges, papaya, mango, kiwi, and red grapes. Good sources of zeaxanthin are yellow corn, squash, mango, honeydew melon, apricots, oranges, kale and peaches.
Antioxidants like, vitamin E and vitamin C, and Omega-3 fatty acids could also help slow AMD. Patients with AMD, whose diet combines leafy vegetables with fish and other high-antioxidant foods, may have a slower progression of age related macular degeneration. Vitamin E is found in eggs, nuts, nut oils, wheat germ, green leafy vegetables, vegetable oils, and whole grains. Omega-3 fatty acids can be found in sardines, tuna, wild salmon, walnuts and flaxseed oil. Vitamin C is found in citrus fruits, strawberries, and cantaloupes and vegetables like tomatoes, leafy greens, yams, and broccoli.
A diet with a high glycemic content may increase the risk of developing macular degeneration. Foods with a high glycemic index include dates, white rice, potatoes, cornflakes, waffles, doughnut, bread and pasta. This means the carbohydrates in these foods are broken down rapidly into glucose or blood sugar and while they can produce a quick energy burst, the deliver little nutrition and low fiber. In high amounts they may damage cells. Foods with low glycemic content are oatmeal, soybeans, yogurt, peanuts, celery, cucumbers, tomatoes, artichokes, broccoli, cauliflower, and spinach.
The National Eye Institute’s (NEI) Age-Related Eye Disease Study (AREDS) found that the following dosage to be beneficial in slowing down macular degeneration:
This may delay or prevent the progressing from intermediate to advanced stage and reduced the risk of vision loss by 25%. There was no benefit found for people with early AMD or people at risk for AMD. Patients with intermediate AMD or advanced AMD(dry or wet) in one eye, but not the other eye, should consider taking the formula.
The National Eye Institute has begun AREDS-2 trials which is focused on studying the effect of the addition of lutein, zeaxanthin and omega-3 fatty acids to the original AREDS formula. Patients in the study will be followed for 5 years and will receive varying amounts of Zinc and beta-carotene.
Always consult a physician before taking any supplements or changing your diet as the AREDS formula may be contraindicated due to other medical conditions or other medications.
What can I do to prevent or slow down loss of vision from macular degeneration?

The Amsler grid is a grid with horizontal and vertical lines used to monitor the central vision of patients with macular degeneration.
Regular eye exams can help diagnose macular degeneration before it causes visual loss or symptoms. During an eye examination, your doctor will check your vision and possibly your refraction, the measurement of the glasses you need. You may also have an Amsler grid described above. An Amsler grid may also be used to help your doctor locate any areas of visual distortion and estimate the severity of the disease. A dilated exam could also be performed as the doctor will look for the presence of drusen and/or mottling of the pigmentation under the macula. If your doctor suspects wet macular degeneration, he/she may choose to do fluorescein angiography. In this procedure, fluorescein vegetable dye is injected into your arm vein and a photographer takes pictures of the retina as the dye travels through its vessels and the choroid (a layer of blood vessels under the retina). Afterward, your doctors can identify very small abnormal vessels and areas of leakage from the vessels, as well as identify areas of pigment changes. Another similar test is indocyanine green angiography which uses a different dye indocyanine green (ICG).
At Eye Physicians Long Beach, an Optical Coherence Tomography (OCT) could also be performed. This noninvasive test uses beams of light to create patterns that can image the retinal cells with resolution less than 10 microns. The OCT will show areas of thickening, areas of thinning, drusen and abnormal fluid under the retina or RPE.