Blog post by: Eye Physicians of Long Beach

Your retina does more work than most people realize. This thin layer of tissue at the back of your eye converts light into the signals your brain turns into images. When something goes wrong with it, vision can deteriorate quickly. Knowing which retinal conditions are most common and what warning signs to watch for can make a real difference in protecting your sight!
What Are Retinal Conditions?
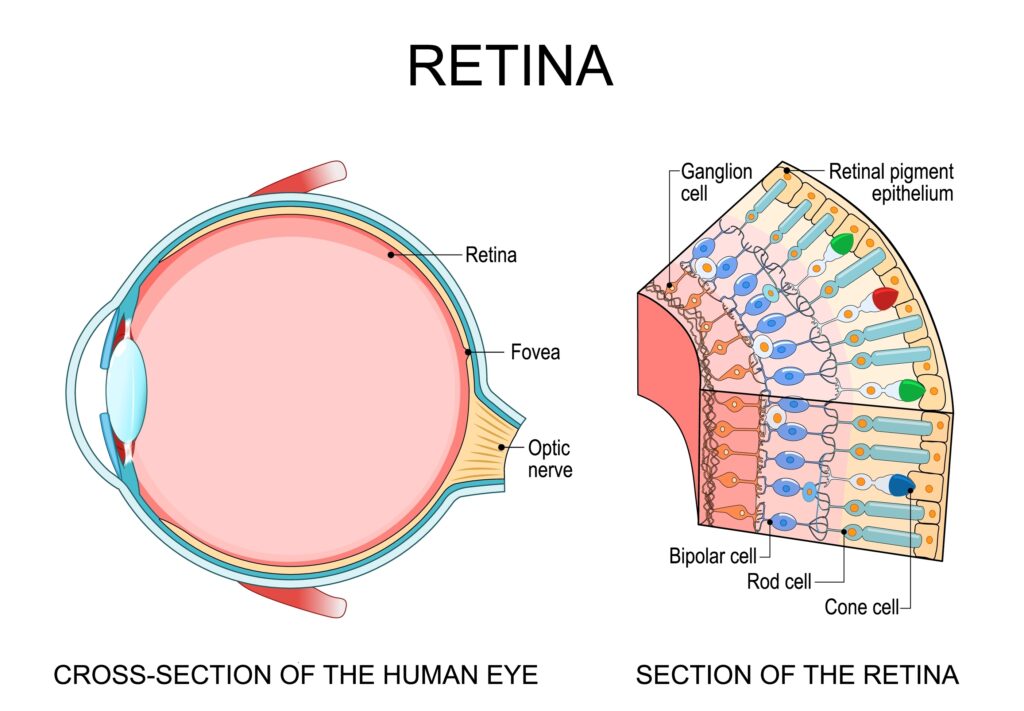
Retinal conditions are diseases or injuries that damage the light-sensing tissue lining the inside of your eye. The retina processes everything you see, including your sharp central vision and your side vision. At its center sits the macula, a small but highly sensitive area responsible for the fine detail you need to read, drive, and recognize faces.
Damage to any part of the retina can blur, distort, or block your vision. When caught early, many of these conditions can be managed effectively. However, left untreated, some retinal conditions can lead to permanent vision loss.
Symptoms and Risk Factors to Know
Retinal problems often announce themselves with noticeable changes in vision. Common warning signs include sudden floaters or flashes of light, blurred or distorted vision, blind spots in your central or side vision, difficulty seeing in dim lighting, and sudden vision loss.
If any of these appear, see an eye doctor right away. Waiting can mean the difference between saving and losing your sight.
Certain factors raise the odds of developing a retinal condition. Diabetes, high blood pressure, severe nearsightedness, and smoking all put added stress on the delicate blood vessels in the retina. Advancing age, a family history of retinal disease, previous eye injuries or surgeries, and long-term use of certain medications such as hydroxychloroquine also increase risk. Knowing where you stand helps you and your doctor stay one step ahead.
The 4 Most Common Retinal Conditions
Flashes and Floaters

Floaters are those tiny specks, threads, or cobweb-like shapes that drift across your field of view. They form when the gel inside your eye (called the vitreous) begins to shrink and clump. Light passing through your eye casts the shadows of these clumps onto the retina, which is what makes them visible.
Flashes happen when the shrinking vitreous tugs on the retina, producing brief streaks or sparks of light, often at the edge of your vision.
Occasional floaters and flashes are usually harmless and become less noticeable over time. A sudden increase in either floaters and flashes appearing together in the same eye, or a shadow spreading across your vision, is a sign that the retina may be torn or detached. This is a situation that needs urgent attention.
Retinal Detachment
Retinal detachment occurs when the retina peels away from the tissue supporting it. As the vitreous shrinks, it can pull strongly enough to tear the retina. Fluid then seeps through the tear, lifting the retina away from the back of the eye. The curtain-like shadow some people notice spreading across their vision is a classic sign, though not everyone experiences it.
Retinal detachment is a medical emergency. Without treatment within hours to days, permanent vision loss in the affected eye is likely. Any sudden change in vision alongside new flashes or floaters warrants an emergency eye exam.
Diabetic Retinopathy
Diabetic retinopathy develops when persistently high blood sugar levels damage the small blood vessels supplying the retina. Those vessels can swell, leak, or close off entirely. In more advanced stages, fragile new blood vessels grow across the retina in an attempt to compensate, but these vessels bleed easily and can cause scarring.
The longer someone has diabetes and the less controlled their blood sugar, the higher the likelihood of retinal damage. Early-stage diabetic retinopathy often has no symptoms at all, which makes regular eye exams particularly important for anyone managing diabetes.
As the condition progresses, anti-VEGF injections and laser therapy can slow its advancement and preserve vision.
Macular Degeneration

Macular degeneration affects the macula, reducing the sharp central vision needed for tasks like reading, driving, and identifying faces.
There are two types of macular degeneration: dry and wet.
The dry form is by far the more common of the two. Tiny protein deposits called drusen build up under the macula, gradually causing it to thin and lose function. Vision loss in dry macular degeneration tends to progress slowly. A specific combination of vitamins and minerals (based on the AREDS2 formula) can help slow that progression in certain patients.
Wet macular degeneration is less common but more aggressive. Abnormal blood vessels grow beneath the retina and leak blood and fluid, which causes rapid scarring and faster vision loss. Anti-VEGF injections, photodynamic therapy, and laser treatment are the main options for managing the wet form.
Protecting Your Vision Starts with Early Detection
Retinal diseases are far easier to manage when caught before significant damage occurs. At Eye Physicians of Long Beach, our ophthalmologists examine the health of your retina at every visit, looking for early changes that might not yet affect your vision. If a problem is found, prompt treatment gives you the best chance of keeping your sight intact.
Has it been a while since your last eye exam? Schedule an appointment at Eye Physicians of Long Beach in Long Beach, CA, today!
